As iron continues to build up in the body, complications happen more often.1
Comparing sickle cell disease patients with iron overload‡ to those without iron overload, a review of clinical trials in 2018 showed that sickle cell patients with iron overload had higher rates of: 3
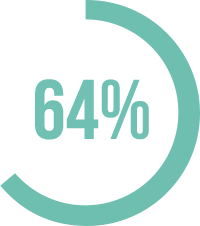
mortality (64% vs. 5%)
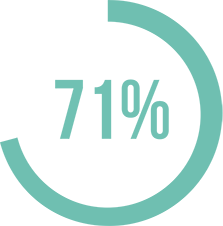
organ failure (71% vs. 19%)
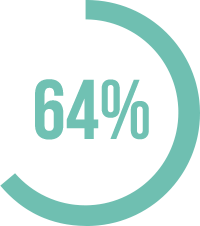
pain episodes (64% vs. 38%)
‡Defined as serum ferritin levels >1,500 ng/mL and transferrin saturation >50% 3
Monitor renal toxicity
Kidney complications are common in patients with sickle cell disease – affecting 30-50% of adults.12 Regular monitoring of both renal and hepatic toxicity can help optimise chelation and ensure patients are on an appropriate chelator.1
Chelation therapy needs to be individually tailored for each patient to respect their lifestyle and to minimise toxicity.1
Iron chelation needs to be adjusted regularly or even switched depending on iron level, weight, and tolerance to side effects.1,2
| Sickle Cell Disease treatment guidelines support regular monitoring of serum ferritin, and cardiac and liver MRI T2*‡1,11 | ||
|---|---|---|
| Parameter | Target | Expert panel recommendation |
| Serum ferritin | 25-300 ng/mL | Monthly |
| Liver iron concentration (LIC) | 800-3,500 µg/g dry weight | Every 1-2 years |
| Cardiac MRI T2* | >20 ms | Performed for patients with:
|
‡Frequency of monitoring and reference values may differ depending on country of practice. Please refer to your local guidelines.
Iron chelation therapy results in better overall survival in sickle cell disease, but only if it is instituted early and compliance is maintained1
For HCP: In case you want to report an adverse drug reaction you become aware of, please report it to your Health Authority according to the requirements set by the pharmacovigilance legislation.